Receiving a diagnosis of metastatic kidney cancer can feel like the ground has shifted beneath your feet. One moment life is ordinary; the next, a doctor is using words like "spread" and "advanced" and your brain is trying to catch up with what any of it means. If you or someone you love is walking this road right now, you are not alone.
Let us start at the beginning.
What Does "Metastatic" Actually Mean?
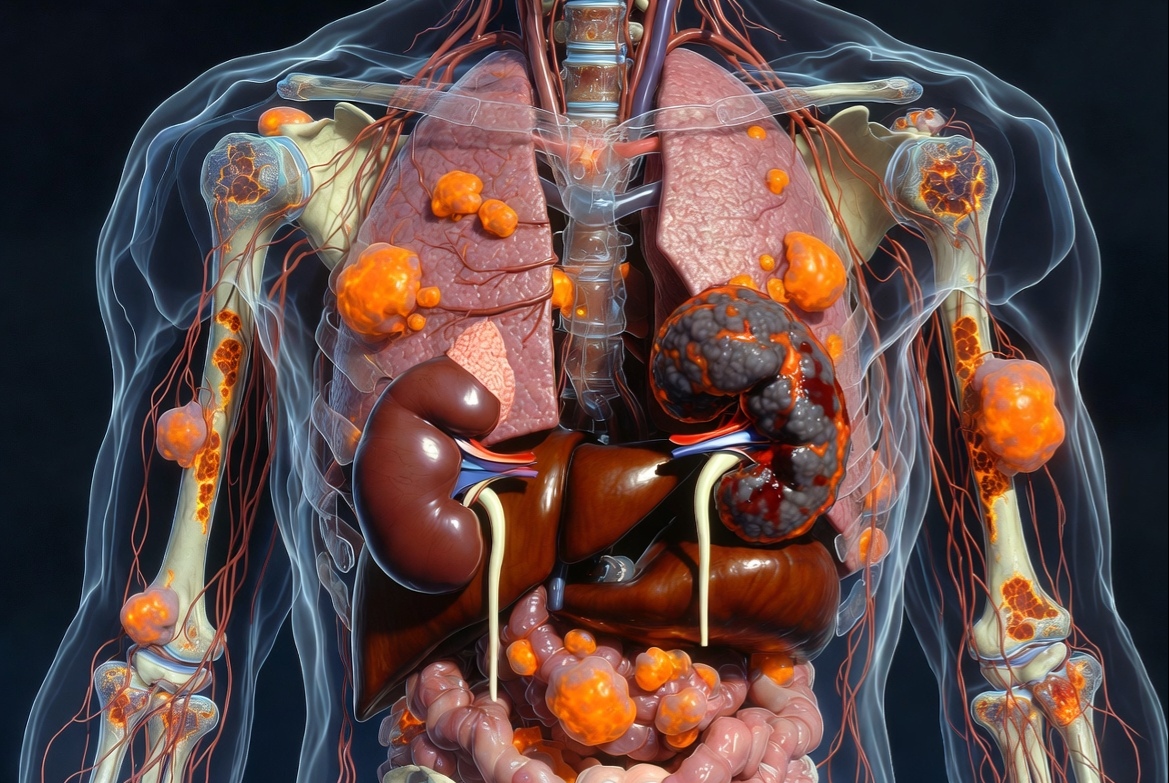
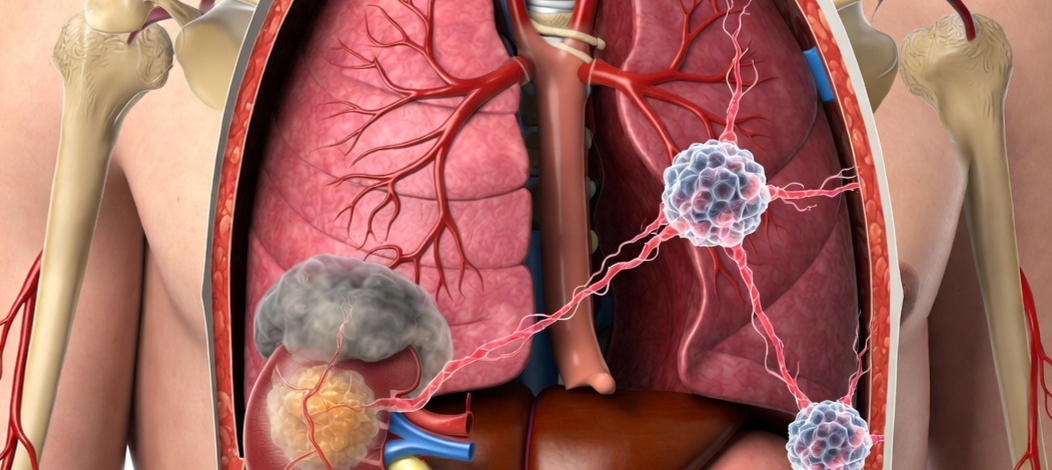
The word "metastatic" simply means the cancer has travelled beyond where it started. In the case of kidney cancer, it began in one or both kidneys but over time, cancer cells broke away, moved through the bloodstream or lymph system, and settled somewhere else in the body. Common destinations include the lungs, liver, bones, brain, and lymph nodes.
This is also called Stage 4 kidney cancer, and whilst it sounds frightening, it is important to understand that metastatic kidney cancer is not the same diagnosis it was twenty years ago. Treatment has changed dramatically, and many people are living for years, not months, with this condition.
Why Does Kidney Cancer Spread So Quietly?
This is one of the most frustrating things about kidney cancer. It rarely causes noticeable symptoms in its early stages. The kidneys are tucked deep inside the body, so a tumour can grow for a long time without causing obvious pain or discomfort. By the time symptoms appear such as blood in the urine, persistent back pain, unexpected weight loss, or a lump in the side, the cancer may have already begun to spread.
That is why a huge number of kidney cancer cases are diagnosed at an advanced stage. It is not that patients ignored warning signs. Often, there simply were none.
Who Is Most at Risk?
Metastatic kidney cancer does not discriminate entirely, but certain factors raise a person's risk. Smoking is one of the strongest known contributors. Obesity and high blood pressure also play a role, as does a family history of kidney cancer. Men are diagnosed roughly twice as often as women, and most cases are found in people over 55, though younger people are absolutely not immune.
Genetic conditions such as Von Hippel-Lindau (VHL) disease can significantly increase the likelihood of developing kidney cancer, sometimes at a much earlier age.
The Most Common Type: Renal Cell Carcinoma
When people talk about kidney cancer, they are usually referring to renal cell carcinoma (RCC), which accounts for around 85% of all kidney cancer diagnoses. Within that group, clear cell RCC is the most prevalent type, and it is also the most studied, which means more treatment options have been developed specifically for it.
Other subtypes include papillary RCC and chromophobe RCC, each with slightly different behaviour and responses to treatment. Knowing your specific subtype matters enormously because it helps your oncologist choose the most effective approach.
How Is Metastatic Kidney Cancer Treated?
This is where the story becomes genuinely hopeful. The treatment landscape for metastatic kidney cancer has been transformed over the past decade, largely thanks to two major advances: targeted therapies and immunotherapy.
Targeted therapies work by blocking specific proteins or pathways that kidney cancer cells rely on to grow. Immunotherapy harnesses the body's own immune system to fight the cancer. Checkpoint inhibitors, particularly drugs that block the PD-1/PD-L1 pathway, have shown remarkable results in some patients, including long-lasting responses. Combination approaches that pair immunotherapy with targeted therapy have become a standard first-line option in many hospitals, showing improved survival times compared to older treatments.
Surgery may also play a role, even in metastatic disease. Removing the primary tumour (a procedure called cytoreductive nephrectomy) can sometimes help, as can surgical removal of individual metastases, particularly when there is only one or a few affected sites.
The key message here is this. Treatment is not one-size-fits-all. Your care team will consider your cancer's subtype, your general health, the locations of the metastases, and your personal preferences before recommending a plan.
Living With Metastatic Kidney Cancer
Living with advanced cancer is both a physical and emotional challenge. Side effects from treatment include fatigue, nausea, high blood pressure, skin reactions, or immune-related inflammation are real and should never be dismissed or silently endured. Always tell your oncologist what you are experiencing. Adjustments can often be made.
Equally important is mental health. Anxiety and depression are common responses to a serious diagnosis, and they are nothing to be ashamed of. Speak to your doctor, ask your oncologist about psychological support, and lean into communities, both online and local, where people truly understand what you are going through.
Questions Worth Asking Your Doctor
If you have been diagnosed with metastatic kidney cancer, come to your appointments prepared. Ask what subtype you have and how that affects your treatment options. Ask whether genomic testing or biomarker testing is available, as this can guide treatment decisions. Ask about clinical trials. Several ongoing studies may offer access to advanced therapies. Also, ask about palliative care, which is not about giving up; it is about managing symptoms and supporting quality of life alongside active treatment.
The Bottom Line
Metastatic kidney cancer is serious. There is no point pretending otherwise. However, it is also a condition that is increasingly manageable, with treatments that continue to improve year upon year. People are living longer, better lives with this diagnosis than ever before.
The most powerful thing you can do, whether you are a patient, a carer, or a loved one, is to stay informed, stay connected, and refuse to face this alone.





Comments (0)
Please sign in to join the conversation.
Loading comments...